Primary ciliary dyskinesia (PCD) is a disorder of the cilia that line the entire respiratory tract, including the middle ear, sinuses, airway, and lungs, as seen in this illustration.
Recall Alert
There is a recall of ibuprofen. Learn more >>
There is a recall of ibuprofen. Learn more >>
Heterotaxy syndrome, also known as isomerism, is a rare condition where many organs in the chest and abdomen are formed abnormally, in the wrong position, or are even missing. Many children with heterotaxy syndrome have complex congenital heart defects (CHD), which often make the condition challenging to treat. The intestines, liver, spleen, and lungs can also be affected.
Some children have a mild form of heterotaxy with only minor abnormalities of just one or two organs. Other children have very complex forms of heterotaxy involving many different organs.
The symptoms of heterotaxy syndrome vary depending on the complexity of heart disease and the involvement of other organs.
Heart symptoms may include:
Gastrointestinal (GI) tract symptoms may include:
Weakened immunity symptoms may include:
Lung and airway symptoms may include:
Heterotaxy syndrome is caused by genetic abnormalities. These abnormalities may be inherited from one or both parents, or they randomly happen. For some children, blood tests can detect a specific gene that may cause heterotaxy, but in many others, a genetic cause can’t be identified.
A positive genetic testing result can help understand a child’s prognosis and risk for complications outside of their heart. It can also be used to understand if other family members are at risk for having the condition and the likelihood that the parents of a child with heterotaxy could have a second affected child.

Check out our downloadable pamphlet for a summary about heterotaxy syndrome. It provides details about the diagnosis, testing, treatment at Boston Children’s, and more.
Congenital heart defects, often involving a combination of the following:
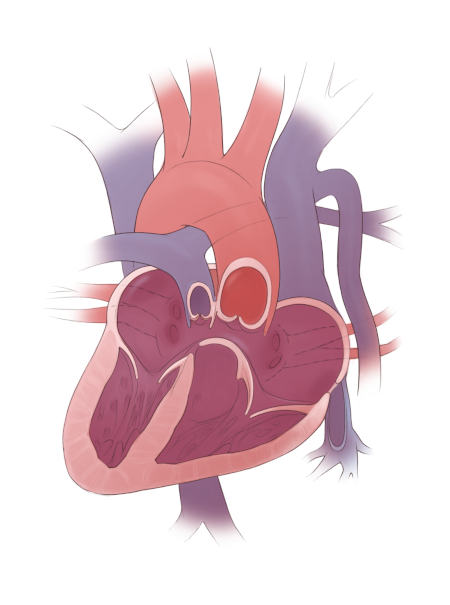
Example of the types of heart defects seen in heterotaxy: dextrocardia, complete atrioventricular canal defect, double outlet right ventricle, pulmonary stenosis, and interrupted inferior vena cava.
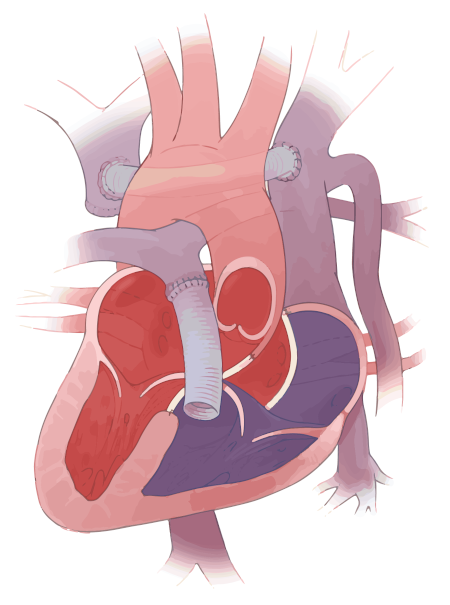
Example of a complete biventricular repair that includes repair of an atrioventricular canal defect and a right ventricle-to-pulmonary artery conduit, and the creation of a neo-innominate vein.
Heart rhythm:
Lungs and airways:

Primary ciliary dyskinesia (PCD) is a disorder of the cilia that line the entire respiratory tract, including the middle ear, sinuses, airway, and lungs, as seen in this illustration.

Normally, the cilia move in an organized and rhythmic way to move mucus up and out of the airway, as seen in this illustration.

In PCD, the cilia can either be malformed or may not work properly, resulting in a build-up of mucus and causing symptoms such as nasal congestion and chronic cough.
Immune system:

Situs solitus, as seen in this illustration, describes normal chest and abdominal anatomy. The illustration also shows the normal position of the lungs, heart, liver, spleen, stomach, and intestines.

The illustration shows heterotaxy with polysplenia, which means multiple spleens are present. Also seen are two left-sided appearing lungs, a heart, midline liver, and stomach. Also illustrated is intestinal malrotation, which may or may not be present in a child with heterotaxy with polysplenia.

The illustration shows heterotaxy with asplenia, meaning the spleen is absent. Also, there are two right-sided appearing lungs, a heart, midline liver, and stomach. Also illustrated is intestinal malrotation, which may or may not be present in a child with heterotaxy with asplenia.

This illustration shows situs inversus, which is the opposite, or a complete reversal, of normal chest and abdominal anatomy. It also shows a mirror-image, or reverse position, of the lungs, heart, liver, spleen, and stomach.
The spleen is often affected in children with heterotaxy, which increases risk of infection. Read about heterotaxy and your child's immune system.
GI tract:
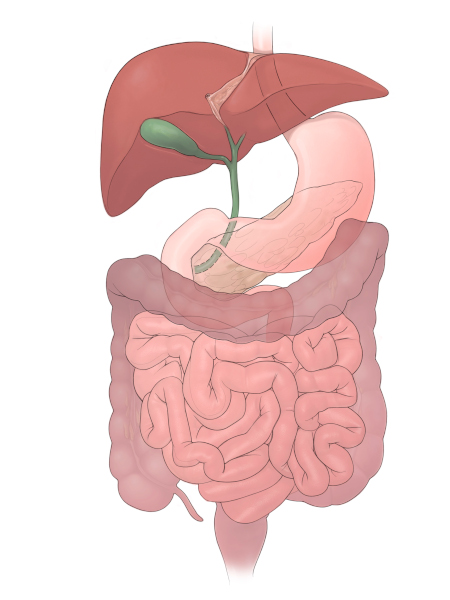
Normal abdominal anatomy
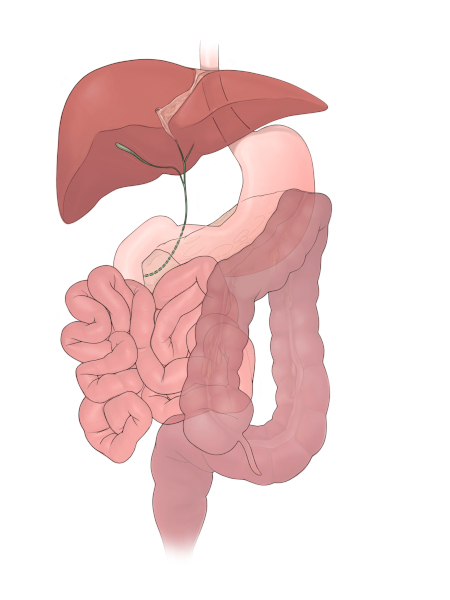
Intestinal malrotation and biliary atresia
Heterotaxy syndrome is diagnosed many different ways. It is often diagnosed before birth, when an ultrasound identifies an abnormal position of one or more organs. Sometimes, it can be diagnosed with a fetal echocardiogram (a special ultrasound of the heart before birth) when a complex heart defect is identified. Also, heterotaxy may be diagnosed during infancy or childhood if your child has feeding problems, breathing problems, cyanosis (blue color), a heart rhythm issue, or a heart murmur.
If heterotaxy syndrome is suspected, your medical team may use the following tests to get a complete picture of your child’s heart and anatomy:
Your child might be screened for other potential health concerns that could be associated with heterotaxy and may need these tests:
Children with heterotaxy syndrome require lifelong follow-up care. The care that your child needs will depend on which systems within the body are affected and the severity. Some children with heterotaxy syndrome who have severe heart defects may need heart surgery shortly after birth to stabilize their circulation. Other children are only mildly affected and may never need surgery.
Children with abnormal cilia may need special inhaled medications to keep their lungs healthy. Those with immune system problems may need daily antibiotic treatment and extra vaccinations to prevent certain infections. Children with malrotation who develop an intestinal blockage may need corrective surgery. Your child’s care team will review test results with you and then develop a treatment plan that is best for your child.

Defying the predictions of local doctors who advised against heart surgery, 6-year-old Faiz’s parents searched the world for a surgeon to treat his complex condition. Now, he’s healthy back home in Pakistan, playing with his siblings and getting ready to participate in sports.
Heterotaxy syndrome can be very complex, and every child’s needs are different. The Heterotaxy Program at Boston Children’s takes a comprehensive approach to treating children with heterotaxy syndrome. We bring together specialists from several disciplines who have extensive experience treating the many conditions associated with heterotaxy.
We screen for and identify potential problems associated with the condition, and collectively create an individualized treatment plan that best addresses the specific complexities of your child’s case. We work together to find treatment solutions for even the most challenging cases. For instance, children with complex heart defects who were previously thought to be candidates for only single-ventricle palliation, or who have already had single-ventricle palliation procedures such as Glenn or Fontan surgeries at other hospitals, might qualify for “two-ventricle” (biventricular) repairs. No matter the type of condition, we will work together to provide a lifetime of care for your child.